Accuity reviews 100% of every inpatient chart before billing with proprietary AI technology.
Physicians and coders then interpret clinical signals to discover the value hidden in your charts.
Where AI accuracy meets physician judgment
Our hybrid approach combines AI precision with physician and coding experts to interpret the gray areas between documentation and coding.
Data received from the health system
Accuity securely receives 100% of each chart's data after discharge.
Powered by physician-governed AI
Amplifi isn’t just smarter on day one. It gets better with every outcome.
- Trained on 7 > million physician-reviewed, payer-adjudicated inpatient charts
- Physician-governed through every step of the process, from design to outcome
- Hundreds of thousands of mapped clinical decision pathways, each leading to a potential DRG opportunity
- Compliant with evidence-based medicine, documentation rules, and coding guidelines
- Continuously improves through a closed-loop learning model grounded in final adjudicated outcomes
Synergy between advanced AI and human clinical and revenue cycle experts
AI Analysis
AI surfacing patterns and gaps at scale
Physician
Clinical lens
Coder
Guidelines and sequencing
CDI Specialist
Documentation integrity
Outcomes-based AI. Multidisciplinary expertise. Exponential results.
Hybrid intelligence finds what AI alone cannot
Accuity is the only AI-driven clinical model that pairs intelligent automation with clinical and revenue cycle expertise.
Amplifi surfaces clinical documentation and coding opportunities everywhere they hide. Then our human experts interpret that complexity, translating clinical reality into precise, defensible codes.
The Accuity model delivers
2-3x
more results than other solutions.
AI finds. Physicians prove. Hospitals keep.
Amplifi surfaces clinical signals and codable clues, and Accuity’s physicians determine and apply the most accurate clinical–coding updates.
Transparent reporting and trend-based education reinforce accuracy over time, helping hospitals deliver predictable ROI dollars and sustained performance at scale.
Recover millions in earned revenue
By uniting clinical integrity with Amplifi AI, Accuity helps health systems capture $4-6 million per 10,000 inpatient discharges.
Improve clinical quality metrics
Accuity improves nationally recognized hospital quality and performance benchmarks including:
- +4.4% in Case Mix Index (CMI)
- +7.6% higher CC/MCC capture
- +10-15% HCC code capture
- Stronger Severity of Illness and Risk of Mortality representation
Prevent and defend denials
By ensuring the final coded record is clinically sound before billing, Accuity helps health systems reduce denials at the source—resulting in lower audit exposure and a sustained 1.5% final DRG-assignment denial rate on reviewed cases.
And when denials do occur, Accuity stands behind its work—providing full support throughout the appeals process.
Accuity is the market leader in delivering sustained, measurable impact at scale.
$4-6M
Cash benefit per 10,000 discharges
2-3x
More than
other solutions
$3.3B
Revenue lift
delivered to clients
1.5%
Final
denial rate
200+
Full time,
U.S.-based physicians
20+
Subspecialties
represented
7M
Charts
reviewed
Reviewing more charts monthly than any U.S. health system
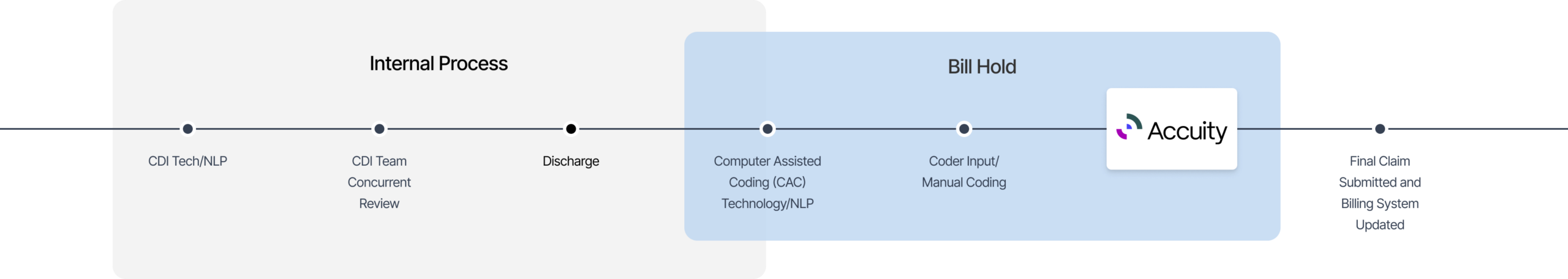
Accuity co-exists across the clinical revenue cycle ecosystem, coming in right before the chart would otherwise go to billing, after your internal CDI process is complete.